Medical simulation
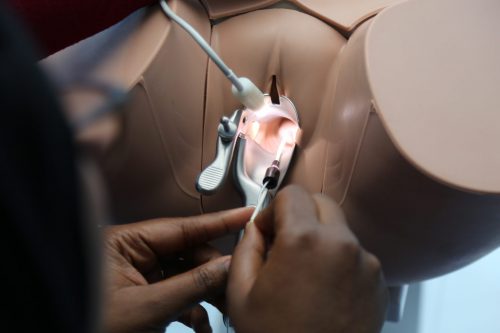
Medical simulation
Simulation is an imitation of a situation or process. Applied to medicine, medical simulation corresponds to the use of synthetic material, virtual reality or standardized patient to reproduce situations that helped to teach (“know-how”) diagnostic and therapeutic procedures or decision-making for healthcare provider.
In 1999, the Institute of Medicine published a report entitled “To err is Human”. Medical errors caused 2-4% of all deaths in the United States . The patient’s safety needs to be improved.
Medical simulation aims to help medical professionals to reduce accidents during general practice, intensive care and surgery.
The evidence-based medicine, called in this context evidence-Based Practice provided for Simulation in Healthcare a high level of evidence.
Two meta-analyses showed the usefulness of medical simulation for nursing education, and teaching medical student . Furthermore, another meta-analysis (including 25 studies), compared the effect of virtual patients to traditional education. It showed similar results for knowledge.
In addition to patient’s safety, medical simulation helped also to standardize training and objective evaluation, reduce cost, increase “Training volume” and improve clinical Efficiency.
In practice, medical simulation is interesting for nurses, medical students, resident physicians, practicing physicians, and also for managers, clerks, technicians, legislators/regulators and multidisciplinary healthcare teams.
Finally, we should retain the maxim “Never the first time on the patient”
MSC mondial
The Medical Simulation Center of the Honoris United Universities network is
+12M
key number
+34K
key number
+280K
key number
Simulation medical
Experiential learning, which draws from prominent scholars such as John Dewey, Jean Piaget, and Carl Rogers, amongst others, underpins simulation-based learning. Often referred to as “learning by doing”, or more broadly, a “theory of experience”, Experiential Learning Theory states that experience plays a central role in human learning & development. The six principles of Experiential Learning Theory align with educational simulation. The six principles are:
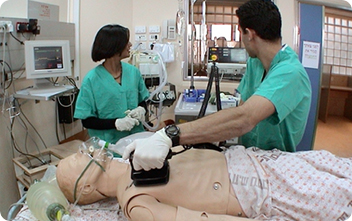
Photo name
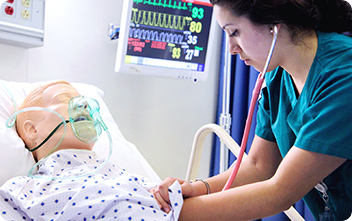
Photo name
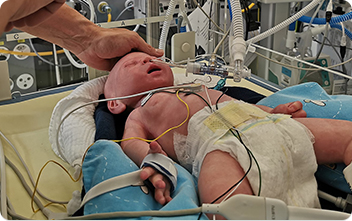
Photo name
Debriefing, & Education Theory
- Engaging students in a process that enhances learning. This includes “feedback on the effectiveness of their learning efforts,” (p. 194) and focus on the process, not the outcome.
- Students have prior beliefs and ideas. A process which draws these beliefs & ideas out, with the intent of re-examining & re-testing them against a topic in order to accommodate new ideas, will lead to learning.
- Learning is a process which cycles between reflection and action, feeling and thinking. “Conflict, differences, and disagreement are what drive the learning process” (p. 194); the resolution of these is what leads to learning.
- Learning happens in interactions between the person and the environment which surrounds them.
- Learning is more than cognition; it also involves thinking, feeling, perceiving, and behaving.
- Learning is grounded in constructivist philosophy; “Learning is the process of creating knowledge
Evidence & Further Study
There exists a paucity of quantitative data regarding the effectiveness of debriefing in medical simulation, despite Lederman’s 1992 seminal Model for the Systematic Assessment of Debriefing. Nearly every article reviewed had a cry for objective studies regarding the effectiveness of debriefing, whether it be comparing: the myriad options of conversational structures, debriefing models, or the comprehensive 5 W’s of Who – debriefer, What – content & methods, When – timing, Where – environment, and Why – theory.[38] Currently, there are critical limitations in the presentation of existing studies, a sparsity of research related to debriefing topics of importance, and debriefing characteristics are incompletely reported.[38][20] Recommendations for future debriefing studies include:
- Duration of debriefing
- Educator presence
- Educator characteristics
- Content of debriefing
- Structure & method of debriefing
- Timing of debriefing[



